What is dental implant osseointegration?
 Winchester dentist Dr Steve Larcombe discusses the importance of osseointegration, a necessary process to ensure the long-term success of dental implant treatment.
Winchester dentist Dr Steve Larcombe discusses the importance of osseointegration, a necessary process to ensure the long-term success of dental implant treatment.
Contents
- Biocompatible and strong
- Surprise discovery
- Jawbone preservation
- Healthy lifestyle = implant success
- Lack of bone
A dental implant is an artificial fixture in the jaw, which acts as a replacement tooth root. It is usually made from titanium. During the placement of an implant, the main aim is to achieve immediate close contact with the surrounding jawbone. After a period of healing, teeth implants become anchored and stable, thanks to osseointegration. This is a process whereby jawbone cells grow up to the implant surface to grip it securely. The word osseointegration derives from the Greek word osteon (bone) and the Latin integrare (to make whole).
Osseointegration occurs over a period of six weeks to six months, depending on the location of the implants and the health of the jawbone. During this time, temporary teeth may be fitted. Once the implants are fully integrated, the permanent replacement teeth are fixed on top of the implants or implant posts.
Implants look, feel and function like real teeth because they provide a solid anchor and supportive root-like structure. The dental implant restoration usually consists of three components. The section replacing the root is a small titanium screw. The titanium roots fuse with the jawbone and provide the foundation for individual crowns, bridges or even a full set of teeth – like a denture. The other two parts of a dental implant are known as the abutment (the connector) and the replacement tooth (the crown).
Biocompatible and strong
Titanium is a metal accepted by the human body and bone cells will easily grow onto its surface. The implant is normally roughened or coated to increase the area available for osseointegration. Titanium is light-weight and biocompatible. It is also a very strong material and can withstand continual biting forces. Titanium is the metal of choice for artificial joints and many other medical procedures.
Surprise discovery
Osseointegration was discovered by a Swedish orthopaedic surgeon, Professor Per-Ingvar Brånemark in 1952. In order to study microcirculation, he had inserted a titanium tube for an optical device into a rabbit’s leg. When he tried to remove the metal tube, Brånemark was surprised to find that he was unable to separate the titanium from the bone. He defined ossesointegration as ‘a direct structural and functional connection between ordered living bone and the surface of a load-carrying implant.’ In 1965, the first titanium dental implants with the intention of osseointegration, were placed in a patient by Professor Brånemark.
Jawbone preservation
Once integrated, dental implants work continually to reduce bone loss and preserve the structure of the jaw. By helping to maintain proper chewing function, implants exert natural forces on the jawbone to keep it functional and healthy. If a gap is left when a tooth is lost, the bone underneath tends to deteriorate due to the lack of chewing stimulation. Bone loss or shrinkage can also occur with natural ageing, injury, gum (periodontal) disease and wearing a conventional denture. The pressure of a denture on the gums during chewing reduces the blood supply, which can also increase the rate at which bone is lost.
Healthy lifestyle = implant success
According to the Association of Dental Implantology, “In general, the success rate for dental implants is around 95 per cent.” Healthy lifestyle choices are essential to successful healing. Smoking restricts osseointegration dramatically and increases the risk that implants may not heal properly after they are placed, making them more likely to fail over time. Nicotine affects blood flow and bone cell growth, two factors essential for osseointegration. A poor diet, excessive alcohol consumption and lack of dental care can also affect the health of dental implants.
Lack of bone
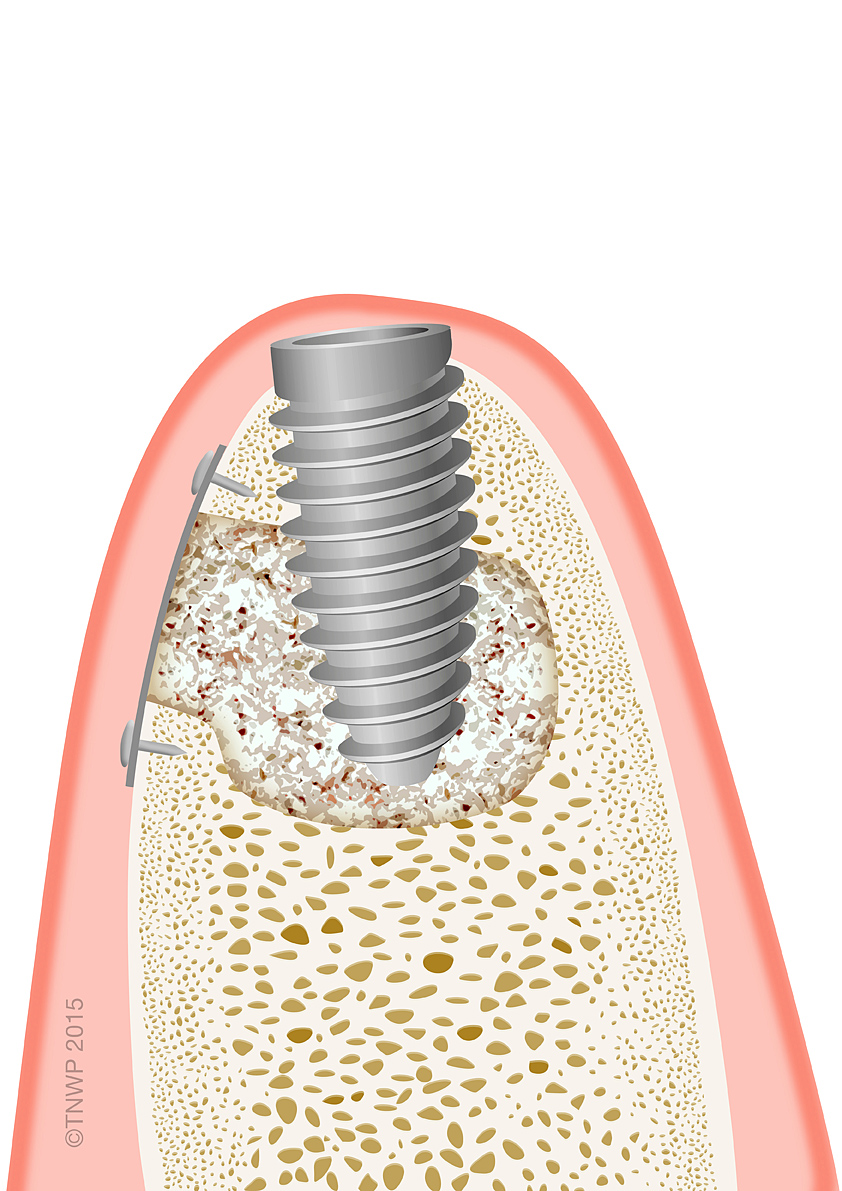
If a patient lacks natural bone in the jaw, it is possible for it to be built up, before implants are placed. Bone augmentation is a term that covers a variety of procedures that ‘build’ bone. This is usually achieved through the use of biologic fillers commonly called bone grafts. Grafting involves the addition of bone to the jaw, to provide a firm base for teeth implants. Bone graft materials can come from a variety of sources: animal, human or synthetic. They all provide a scaffold into which new bone will grow.
If you are considering dental implant treatment, understanding how implants integrate with your jawbone can help provide peace of mind. Find out if dental implants are right for you.
About the author - Dr Steve Larcombe practises at Winchester Dental Implant Centre. Steve is skilled in surgical techniques and has been providing dental implant treatment for more than 25 years. His practice provides a full and comprehensive range of dental implant services, with an emphasis on high quality and prevention of further dental disease. Dental implants and fixed or removable teeth with localised or extensive bone augmentation are provided in a pain-free environment.
